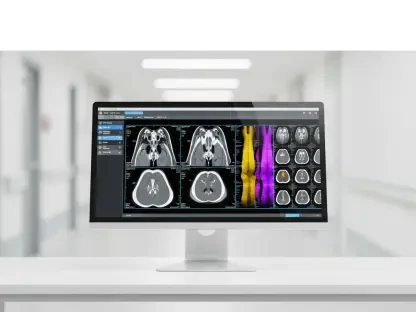
The healthcare landscape in the United Kingdom has reached a precarious tipping point where approximately half a million medical images remain unreported beyond the standard twenty-eight-day target. This staggering backlog is not merely a statistical anomaly but a symptom of a deeply rooted systemic failure within the diagnostic infrastructure that supports millions of patients. As clinicians face an unprecedented surge in demand for complex imaging, the promise of artificial intelligence as a silver bullet has begun to lose its luster. Instead of liberating radiologists from the drudgery of routine analysis, these digital tools often act as a secondary burden, demanding additional validation and documentation that the current workforce simply cannot afford to provide. The crisis is compounded by a demographic shift that sees seasoned experts exiting the field at an alarming rate, leaving behind a void that no algorithm, regardless of its processing power, is currently equipped to fill in the immediate future.
The Expanding Gap: A Workforce Under Unprecedented Pressure
The structural integrity of the radiology sector is currently undermined by a thirty percent shortfall in clinical radiology consultants, a deficit that is projected to widen to nearly forty percent by 2029. This workforce erosion is driven by more than just a lack of new recruits; it is accelerated by a troubling trend of early retirement among the existing staff. Many highly skilled consultants are choosing to depart the profession at a median age that has recently plummeted toward forty-five, citing chronic exhaustion and a feeling of being undervalued. This “brain drain” means that the remaining clinicians must absorb an ever-increasing volume of diagnostic work, which includes complex MRI and CT scans that require nuanced interpretation. Without a massive influx of human talent, the system remains fragile, and the reliance on technological patches appears more like a temporary bandage than a sustainable cure for a sector that is fundamentally understaffed.
When analyzing the operational reality of the NHS, the consequences of this shortage manifest in a persistent backlog of roughly five hundred thousand scans every year. These delayed reports represent hundreds of thousands of patients waiting for critical diagnoses that could dictate the course of their treatment for cancer or cardiovascular issues. The pressure to clear these stacks of data often leads to a cycle of burnout where radiologists are pushed to their cognitive limits, increasing the risk of diagnostic errors. Paradoxically, the introduction of high-tech solutions was intended to mitigate this risk, yet the reality in the reading room is far different. Experts frequently compare the deployment of advanced software in such an environment to trying to install smart lighting in a house that is already engulfed in flames. The fundamental issue is not a lack of sophisticated sensors or automated switches but the lack of a solid structure to support them.
The Efficiency Paradox: When Technology Adds to the Load
While artificial intelligence is often marketed as a productivity enhancer, recent data suggests a contrary effect, with nearly thirty-seven percent of clinical directors reporting that these tools actually increase their daily workload. A primary culprit in this efficiency drain is the high rate of false positives generated by even the most advanced computer-aided detection systems. For example, software designed to identify lung nodules might flag nine false positives for every one true positive finding. Because clinical standards and professional liability require a radiologist to meticulously document and explain why each AI-suggested finding is rejected, the process often becomes more time-consuming than if the human expert had simply performed a manual review from the start. This digital “noise” creates a bottleneck where clinicians are forced to act as editors for an algorithm rather than focusing their specialized expertise on complex cases.
The lack of seamless integration into local workflows has led to a high rate of technological abandonment, with approximately thirty-five percent of AI-assisted tools being discarded within eighteen months of their implementation. These failures often stem from software being developed in a vacuum, without a deep understanding of the demographic variations or the specific hardware configurations present in diverse clinical settings. When a tool is not calibrated to the local patient population, its accuracy drops significantly, leading to the aforementioned surplus of false alerts. Furthermore, the administrative overhead required to manage these systems often outweighs the marginal gains in diagnostic speed. For technology to truly serve the medical community, it must be designed as an extension of the radiologist’s existing environment rather than a standalone disruption that requires constant troubleshooting and manual oversight by the already exhausted medical staff.
Legal Vulnerabilities: Redefining Responsibility in a Digital Era
Beyond the immediate logistical challenges, the adoption of diagnostic software introduces a complex layer of legal risk that many practitioners find deeply concerning. Research involving mock jurors revealed a significant trend: radiologists were much more likely to be found liable for malpractice if they relied on AI feedback without conducting a redundant assessment of the original scan. To mitigate this legal exposure, many doctors have adopted a double-work strategy, reviewing the images entirely on their own before even looking at the machine’s suggestions. This defensive medicine approach effectively negates any potential time savings the technology might have offered, as the human professional essentially performs the same task twice to ensure they are protected in court. The fear of litigation in an environment where liability frameworks remain unclear creates a psychological barrier that prevents the effective collaboration between human intelligence and machine learning.
The consensus among medical and technological experts established that a unified strategy prioritizing the human element over software installation was the only viable path forward. It was determined that successful implementation required a shift away from isolated tool development toward a model that integrated AI into existing platforms with localized demographic data. Researchers found that technology functioned best as a secondary support system rather than a primary diagnostic driver, provided that workforce growth was also aggressively pursued to reduce baseline burnout. The legal community began to recognize that liability standards needed to evolve, suggesting that clear protocols for human-AI interaction could reduce the need for redundant workflows. Ultimately, the industry concluded that the most effective solutions were those that empowered clinicians to spend more time with patients and less time managing inaccurate digital flags and complex software.