Across Thailand’s hospitals and labs, a quiet revolution in healthcare AI is hitting critical mass as developers, clinicians, and policymakers align incentives to automate care and rewire operations at scale. The fastest-growing cohort in the country’s tech economy now sits inside health systems and robotics teams, where AI touches clinical workflows from triage to sterile corridors navigated by autonomous machines. The momentum did not appear overnight. Policy certainty set the pace, capital followed, and real deployments seeded a new labor market that blends model training, safety engineering, and compliance. Yet the path is not frictionless. Brain drain, data silos, spiraling compute budgets, and a fragile trust compact with patients all weigh on execution. Whether Thailand turns a national ambition into regional leadership depends on how deftly it converts strong demand signals into repeatable, compliant systems that improve outcomes while protecting privacy.
Policy Tailwinds and Investment Momentum
Government signals have reframed risk for investors weighing long-term bets on clinical AI and digital infrastructure. The Board of Investment’s refreshed measures for 2026–2027 include as much as eight years of corporate income tax holidays for projects in AI, data centers, and wellness-linked digital services. That incentive stack narrows payback periods for capital-heavy platforms, from medical imaging models to privacy-preserving analytics. It also supports “sovereign AI” ambitions: localized data pipelines, Thai-language models, and in-country compute arranged to meet data residency expectations. With a THB 25 billion National AI Programme approved in mid-2025, procurement clarity improved, enabling hospitals to operationalize pilots rather than stall in proof-of-concept limbo.
Hiring trends mirrored the capital shift. Health tech investment climbed to about $420 million, a 133% rise over two years, while Smart Visa issuances reached roughly 5,800, up 176% in the same period. The developer base swelled as well: active healthcare AI practitioners expanded to around 28,500, reflecting a 137% jump. These figures matter because they push the market from adoption to production, where model governance, audit trails, and post-deployment monitoring become the norm, not an afterthought. However, policy alone cannot conjure talent. The country still graduates only a few hundred AI engineers annually, far short of the tens of thousands needed. As a result, BOI-backed projects now pair tax relief with aggressive hiring of mid- and senior-level specialists, often recruiting across borders to plug near-term gaps.
Physical AI Moves From Labs to Wards
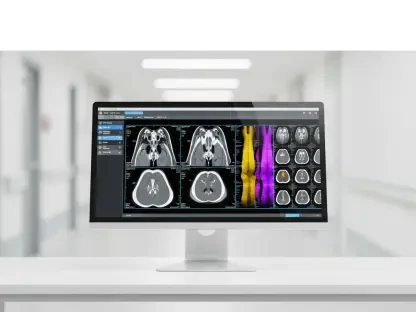
Robotics has shifted from exhibition floors to live clinical environments, moving beyond telepresence carts to autonomous systems with defined safety cases. At King Chulalongkorn Memorial Hospital and partner sites, robots such as HAPPY and CORGI—developed by True Digital in concert with university labs—now handle tasks that borrow from both industrial autonomy and clinical caution. They map corridors, open doors, and use image-based inference to estimate radiation levels, dramatically reducing staff exposure during radioactive iodine treatments. In tuberculosis isolation areas, autonomous delivery reduces cross-contact, supporting infection control protocols while freeing nurses for higher-value work. Each capability stacks on the last, converting isolated pilots into a “digital intelligence fabric” that coordinates machines, cloud services, and hospital information systems.
Building on this foundation, demographics have turned physical AI from an intriguing option into a practical necessity. Thailand’s aging population has pushed hospitals to scale remote vitals monitoring, fall-risk prediction, and medication adherence checks, where device telemetry and machine learning close staffing gaps without compromising safety. In this context, robotics development demands cross-disciplinary teams: control engineers who write safe motion primitives, perception experts who fuse depth sensors with LIDAR, and ML specialists who tune models for messy, real-world data. Systems integrators handle interfaces to electronic medical records and pharmacy systems, while safety engineers run failure-mode analyses aligned to medical standards. The cumulative effect is an employment flywheel that extends well beyond traditional software roles.
The Talent Market Is Rewiring
As deployments matured, employers rewrote job descriptions to prioritize hybrid fluency—technical depth plus clinical, regulatory, and data stewardship literacy. Three roles led the surge. Bio-Data Architects reshape chaotic clinical data into standardized, de-identified corpora, stitching EMR fields, imaging archives, and sensor feeds into training-ready datasets under privacy controls. Robotics Integration Specialists bridge AI software with medical-grade hardware, ensuring perception pipelines align with control loops and that robots interoperate with hospital systems. AI Compliance Officers map models to local and international regulations, validating performance, managing audit trails, and enforcing consent flows. Each function grew by more than 50% year over year, reflecting the shift from “using AI” to “building AI” with healthcare-grade rigor.
Sovereign AI ambitions intensified that shift, especially for language-first applications addressing patient communication and clinician documentation. Developers increasingly fine-tune large language models to handle Thai and regional dialects, elevate medical terminology coverage, and respect cultural nuance in elder care. Teams now include linguists and data curators who construct specialized corpora—discharge summaries, lab reports, consent scripts—paired with red-team evaluators who test for hallucinations and bias. Hospitals are also rolling out retrieval-augmented generation against localized knowledge bases to anchor outputs in verified guidelines. This approach improved trust and accuracy while reducing dependence on foreign models that underperform in Thai contexts. The result is not only better bedside communication but also a stronger domestic capability in model governance.
Proof Points and Patient Trust
Real-world evidence has accumulated, cutting through hype with measurable outcomes. King Chulalongkorn Memorial Hospital’s “digital intelligence fabric” links cloud-hosted inference, robotics fleets, and hospital applications into a cohesive operational layer. Robots execute door-opening routines with tactile feedback, flag elevated radiation zones using camera inference, and deliver drugs in sealed containers with chain-of-custody logs. On the software side, scheduling models predict no-show risk based on appointment history and travel data, triggering outreach in Thai and regional dialects. Imaging AI assists rural clinics by prioritizing suspected pneumothorax or stroke cases from X-rays and CT scans for rapid review in urban centers, shortening time-to-intervention for patients who would otherwise wait hours or days.
However, scale depends on a workable trust compact. Public awareness of AI is high, but only a small slice of consumers behaves like full-potential users. Design teams have responded with clearer consent flows, straightforward risk disclosures, and explainable outputs that read like clinical notes rather than black-box scores. Ethical AI specialists test for demographic skews and monitor drift in production, while UI/UX leads craft interfaces that fit clinician routines—no tiny fonts, no modal pop-ups during critical tasks, and no alerts that lack clear mitigation steps. Hospitals also pilot privacy-preserving ML methods for federated learning across facilities, reducing the need to centralize sensitive data. The message is subtle but consistent: AI should feel like a responsible aide, not an inscrutable authority.
The Road Ahead: Constraints, Next Steps, and Outcomes
Even with favorable policies, several bottlenecks constrained the pace of change. Brain drain continued to siphon senior talent to Singapore and Silicon Valley, outpacing wage growth at home. Fragmented data and legacy IT slowed aggregation, forcing teams to budget months for schema mapping and quality checks before training. Security anxieties persisted amid reports of healthcare breaches regionally; with a majority of consumers worried about fraud or hacking, providers invested in security engineering and privacy reviews as precursors to deployment. Compute remained expensive for large medical imaging models and Thai language models tuned for clinical use, prompting selective training strategies, transfer learning, and partnerships with regional data centers to keep latency and costs in check.
Given these constraints, actionable priorities were clear. Hospitals that standardized data schemas and built MLOps pipelines captured operational gains earlier and de-risked multi-site rollouts. Investors that paired BOI incentives with rigorous compliance and cybersecurity built stronger partnership pipelines with top hospital networks. For job seekers, cross-disciplinary depth—data engineering plus clinical ontologies, robotics plus safety certification, ML plus regulatory technique—proved decisive. Policymakers leaned on Smart Visas to import expertise while accelerating domestic upskilling. As these steps took hold, Thailand advanced from pilots to scaled operations in tertiary centers and began exporting service models to neighbors. The path forward demanded persistence, but the combination of policy clarity, physical AI maturity, and language-first modeling had already translated into tangible, patient-facing improvements.